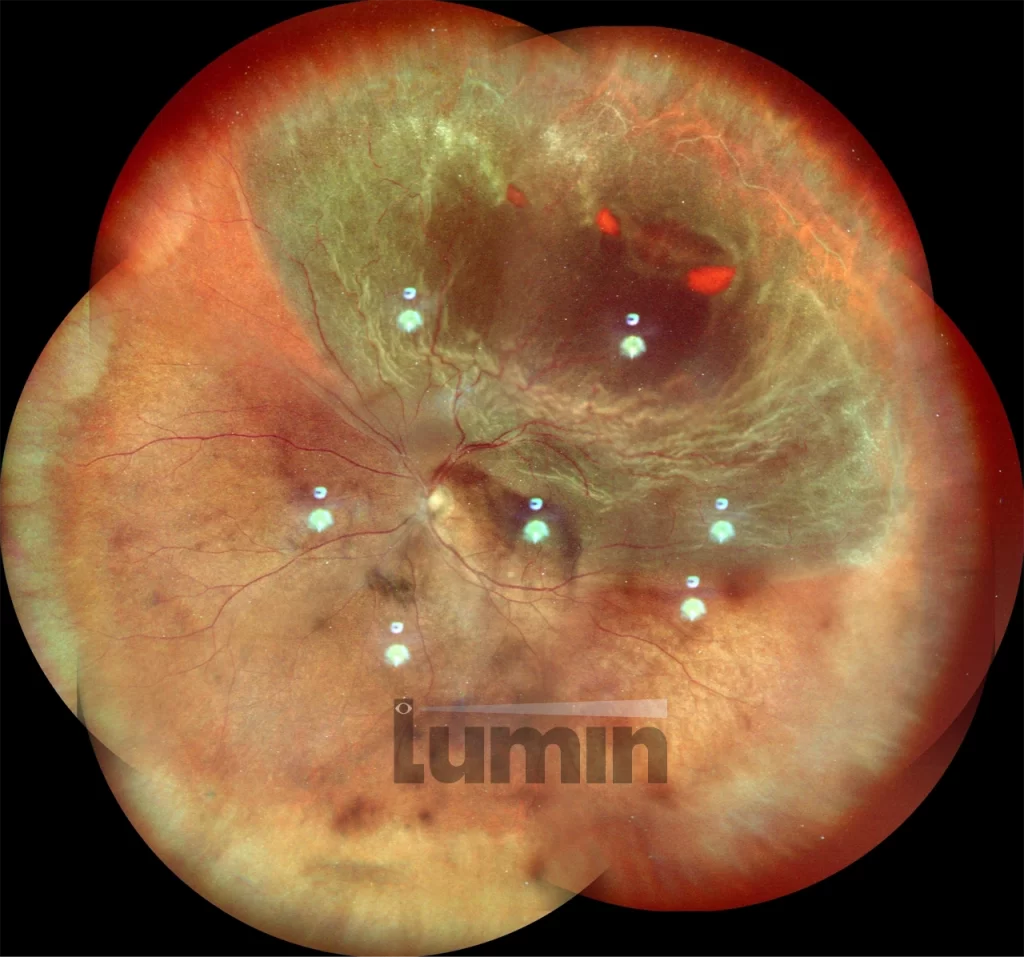
The retina is a light sensitive structure at the back of the eye that receives the images we see. Retinal detachment is an emergency. Delay or failure to treat a retinal detachment will lead to permanent loss of vision.
Retinal detachments often follow a retinal tear. The retinal tear acts as an opening allowing fluid to go behind the retina, causing the retina to separate from the wall of the eye.
If you experience any of these symptoms, seek immediate medical attention from an ophthalmologist or retina specialist in Singapore. Prompt diagnosis and treatment are vital to prevent permanent vision loss.
During the examination, your eye care professional will dilate your pupils for a better view of the retina. They may use specialised imaging techniques, such as optical coherence tomography (OCT) or ultrasound to evaluate the retinal detachment.
Treatment for retinal detachment usually involves surgery. The type of procedure would depend on the characteristics and severity of the detachment. There are three main surgical techniques used:
The vitreous gel is removed using small instruments followed by flattening of the retina and laser therapy to seal the retina breaks. This is often combined with the introduction of a gas or silicone oil to hold the retina in place for a few weeks to months to improve the success of the surgery. Posturing may be required for a few weeks after the surgery.
This involves the placement of a supportive device (scleral buckle) to the external wall of the eye to encourage the reattachment of the retina. Laser and/or cryotherapy treatment is applied to the retinal tear to seal the break.
This procedure involves inserting a gas bubble into the eye to push the detached retina against the back wall of the eye. Laser or cryotherapy is then used to seal the retinal tear or hole. Dedicated posturing after the procedure is required to achieve success.
Treatment for retinal detachment usually involves surgery. The type of procedure would depend on the characteristics and severity of the detachment. There are three main surgical techniques used:
Laser photocoagulation or cryotherapy is often used to seal a retinal break or tear and prevent fluid from accumulating beneath the retina. In cases where the detachment is small and located away from the macula—the central area responsible for sharp vision—laser treatment can be used to isolate the affected area and stop the detachment from progressing.
Vitrectomy involves removing the vitreous gel—the clear, jelly-like substance inside the eye—to eliminate any pulling forces on the retina. This procedure is chosen based on the location and nature of the retinal tear or if there are tractional membranes present. During the surgery, small incisions are made in the sclera, fluid under the retina is drained, and laser treatment is applied to seal the break. At the end of the procedure, a gas bubble or silicone oil may be introduced into the eye to keep the retina in place. If silicone oil is used, a second surgery is needed to remove it. If gas is used, it will naturally absorb over a few weeks. Post-operative positioning may also be necessary to improve the success rate.
This procedure involves placing a flexible band, usually made of silicone, around the outside of the eye to gently press the eyeball’s wall inward. This supports the area of the retinal break and helps relieve tension caused by the vitreous gel. Cryotherapy is often applied during the surgery to seal the tear. Sometimes, air or gas is injected into the eye to hold the retina in place. After surgery, patients may be advised to maintain a specific head position for several days to support healing.
This technique involves injecting a gas bubble into the eye to press the retina back into place. Laser or cryotherapy is then used to seal the break. Pneumatic retinopexy is suitable for specific types of retinal detachments, typically those caused by tears in the upper (superior) part of the retina. Success relies heavily on strict head positioning after the procedure.

Expertise matters when managing complex retinal conditions. At Lumin Eye Specialists, our retina specialist offers years of experience and a deep understanding of retinal diseases. Our comprehensive approach covers everything from routine screenings to surgical interventions for retinal detachments and other related disorders.
Dr Clarissa Cheng is trained in medical and surgical retinal care, detecting early retinal tears and managing complex detachments. We use diagnostic and surgical equipment, ensuring precise evaluations and tailored Treatments.
If you have a retinal condition, book an appointment with our specialist.
The retina, commonly described as the film of the eye, is the light-sensitive layer responsible for capturing images and transmitting them to the brain through the optic nerve. Retinal detachment occurs when the retina becomes lifted or separated from its normal position. This separation disrupts its function and begins to compromise the health of the retinal tissue. If not treated promptly, retinal detachment can result in permanent vision loss.
There are three main types: rhegmatogenous, tractional, and exudative. Rhegmatogenous is the most common, caused by a tear in the retina.
There are many causes of retinal detachment but the most common cause is a retinal hole or tear. This allows fluid in the eye to go underneath the retina causing it to come off.
A person may experience a sudden appearance of floaters, flashes of light, or ‘cobweb-like’ shapes in their field of vision. If these symptoms were already present, there might be a noticeable increase—either sudden or gradual—in their number or intensity. Additionally, some individuals may notice a sensation of a “curtain” or shadow descending over part of their vision. This shadow can spread and may eventually lead to a loss of central vision.
Retinal detachment occurs in approximately 1 out of every 10,000 to 15,000 individuals. Risk factors for retinal detachment include aging, trauma, severe myopia, family history of retinal detachment, and previous eye surgery.
If you are at risk for retinal detachment, it may be advisable to avoid activities that involve sudden or forceful eye movements, such as contact sports or roller coaster rides. Regular eye check-ups can help detect retinal tears or breaks early, and timely laser treatment can lower the risk of progression to retinal detachment.
If you do not treat a retinal detachment, yes, it can lead to permanent vision loss, including complete blindness in the affected eye.
Here’s why:
Key Points:
If you suspect a retinal detachment or are experiencing symptoms (like flashes, floaters, or a shadow over your vision), it’s important to see an eye specialist immediately — this is considered a medical emergency.
There are several methods available to repair a retinal detachment. The choice of treatment depends on the type and severity of the detachment. A retinal specialist will determine the most appropriate approach, and in some cases, a combination of techniques may be used to improve surgical outcomes and increase the success rate.
Treatment options include laser surgery, cryopexy, pneumatic retinopexy, and scleral buckle surgery, depending on the type and severity.
Surgical treatments for retinal detachment are successful in over 90% of cases in terms of reattaching the retina to the eye wall. However, more complex cases may require a combination of techniques or multiple surgeries for optimal results.
Vision recovery varies depending on several factors, with the most important being whether the macula - the most sensitive part of the retina - was detached, the severity of the detachment, duration of detachment, and any co-existing eye problems. Some patients regain full vision, while others may experience partial recovery. Early treatment improves outcomes. The longer the retina stays detached, the greater the risk of permanent vision loss.
Before Your Operation
Before your operation your doctor or nurse will take a detailed medical history, including any medications you are currently taking. Please prepare your list of medications. You may also need to undergo tests such as blood work and an ECG to ensure you are medically fit for the procedure.
If cataract removal is planned as part of your surgery, additional measurements will be taken to determine the correct lens implant needed for successful visual outcomes.
At this appointment, we will also explain the surgical procedure in detail and answer any questions you may have. Additionally, we will review your medications and provide guidance on whether any need to be stopped prior to surgery, particularly blood thinners and medications used to manage diabetes.
What to Expect on the Day of Surgery
You will receive specific instructions about when to stop eating and drinking before your operation. Depending on the scheduled time of your surgery, you will be asked to arrive either early in the morning (for morning procedures) or later in the morning (for afternoon procedures).
In most cases, an overnight stay in the hospital is required, so we recommend bringing a small overnight bag with toiletries and a change of clothes.
Please be aware that retinal detachment surgery may sometimes need to be performed as an emergency, depending on the urgency of your condition.
You will receive specific instructions about when to stop eating and drinking before your operation. Depending on the scheduled time of your surgery, you will be asked to arrive either early in the morning (for morning procedures) or later in the morning (for afternoon procedures).
In most cases, an overnight stay in the hospital is required, so we recommend bringing a small overnight bag with toiletries and a change of clothes.
Please be aware that retinal detachment surgery may sometimes need to be performed as an emergency, depending on the urgency of your condition.
After your surgery, your operated eye will be covered with a protective plastic shield held in place with tape. The following day, a nurse will remove the shield, gently clean your eye, and administer the prescribed eye drops. You and your family members will also be shown how to correctly apply the eye drops and given guidance on proper eye care at home.
You may experience some temporary side effects from the local anaesthetic, such as numbness on one side of your face, a mild headache, or double vision. These effects usually wear off within 1 to 2 days.
It’s normal to have some redness, swelling, drooping of the eyelid, and a gritty or irritated feeling in the eye for up to 4 weeks after surgery. Mild discomfort can usually be managed with pain relief medication. However, if you experience severe pain—especially if it’s accompanied by headache or vomiting—seek medical attention immediately.
Your vision will likely be blurred after surgery, particularly if a gas or oil bubble was used inside the eye. Vision will gradually improve as the gas is absorbed or after the oil is removed. The final level of vision depends on the condition and recovery of your retina.
After your surgery, you will need to remain in the recovery area for 1 to 2 hours until you are fully awake and stable. Depending on the type of surgery performed, the type of anaesthesia used, and your overall medical condition, an overnight hospital stay may be recommended.
As your vision will be temporarily blurred in the operated eye, we strongly advise arranging for someone to accompany you and assist you in getting home safely.
You may need to maintain a specific head position following surgery, especially if a gas bubble or silicone oil has been placed inside the eye. Proper positioning is crucial to support the healing process and improve the outcome of your surgery.
Important Guidelines:
To promote healing and prevent complications after your eye surgery, please follow these care instructions carefully:
Over the next six weeks, you can expect your eye to become more comfortable, with reduced swelling and redness. Depending on your eye’s condition, your vision should gradually improve over the following 3 to 6 months. Your retinal specialist will slowly reduce your eye drops, and in some cases, stitches (sutures) may be removed.
For a detailed eye assessment or personalised recommendations on treatment, reach out to us – We look forward to bringing back the light into your life.
Bus services (bus stop 13019): 7, 75, 77, 105, 106, 123, 174, 174E
For more information on shuttle services and parking, please refer to this link (https://www.gleneagles.com.sg/plan-your-visit/getting-here).